November 26, 2012
November 20, 2012
Neurosky's PuzzleBox Orbit
 |
Puzzlebox Orbit: A brain-controlled helicopter blending science, education, and open source
|
The
Puzzlebox Orbit is operated via a NeuroSky EEG headset plus either a
mobile device or the dedicated Puzzlebox Pyramid remote. Users can fly
the Orbit through focused concentration or by maintaining a state of
mental relaxation. What makes the Puzzlebox Orbit truly unique however
is the open release of all source code, hardware schematics, 3D models,
and step-by-step building instructions which are published freely online.
Puzzlebox
Orbit features a unique spherical design that protects helicopter
blades from unintended impact with objects such as walls and ceilings,
while lending a pleasantly technical aesthetic.
The Kickstarter:
After
two years of development and a Guinness World Record (in collaboration
with NeuroSky), Puzzlebox has completed funding on its first consumer
hardware product via Kickstarter.
Puzzlebox
is building and selling a MindWave and MindWave Mobile compatible
helicopter. They will sell finished, working, brain-controlled
helicopters AND release guides and software for taking them apart to
rebuild or customize. Puzzlebox publishes lessons on how mind-controlled
devices actually work and how infrared signals steer the aircraft. The
hypothesis is that this form of cooperation can succeed commercially
while aiding the pursuit of science and education.
Puzzlebox and NeuroSky's overall goal with this project is to explore an Open approach to Brain-Computer Interface
(BCI ) technology. Advances at the cutting edge are waiting to find
their way to the public and this project is our latest contribution.
November 13, 2012
Modeling pulmonary edema in a lung-on-a-chip
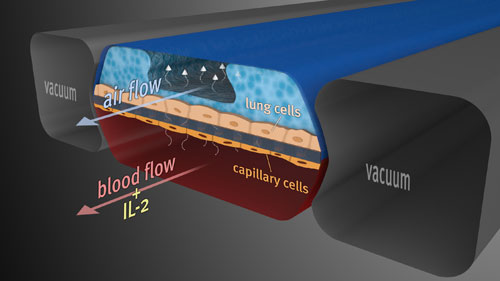
The
Wyss Institute’s human breathing lung-on-a-chip, made using human lung
and blood vessel cells, acts much like a lung in a human body. A vacuum
re-creates the way the lungs physically expand and contract during
breathing. In the current study, when researchers applied the cancer
drug IL-2, fluid from the bottom of the chip entered the air channel on
the top, and the blood clotted — mimicking what happens when humans get
pulmonary edema. Further, when they turned on the vacuum to simulate
breathing, the fluid leakage was much worse — adding new insight to what
scientists understand about this life-threatening condition. (Credit:
Donald Ingber et al./Wyss Institute)
Researchers at the Wyss Institute for Biologically Inspired Engineering at Harvard University have mimicked pulmonary edema in a microchip lined by living human cells. They used this “lung-on-a-chip” to study drug toxicity and identify potential new therapies to prevent this life-threatening condition.
The study offers further proof-of-concept that human “organs-on-chips” hold tremendous potential to replace traditional approaches to drug discovery and development, according to the researchers.
“Major pharmaceutical companies spend a lot of time and a huge amount of money on cell cultures and animal testing to develop new drugs,” says Donald Ingber, M.D., Ph.D., founding director of the Wyss Institute and senior author of the study, “but these methods often fail to predict the effects of these agents when they reach humans.”
The lung-on-a-chip device, which the team first described only two years ago, is a crystal-clear, flexible polymer about the size of a memory stick that contains hollow channels fabricated using computer microchip manufacturing techniques.
Two of the channels are separated by a thin, flexible, porous membrane that on one side is lined with human lung cells from the air sac and exposed to air; human capillary blood cells are placed on the other side with medium flowing over their surface. A vacuum applied to side channels deforms this tissue-tissue interface to re-create the way human lung tissues physically expand and retract when breathing.
Wyss Technology Development Fellow Dongeun Huh, Ph.D., who also holds appointments at Boston Children’s Hospital and Harvard Medical School, studied a cancer chemotherapy drug called interleukin-2 — or IL-2 for short — in the lung-on-a-chip. A major toxic side effect of IL-2 is pulmonary edema, which is a deadly condition in which the lungs fill with fluid and blood clots.
When IL-2 was injected into the blood channel of the lung-on-a-chip, fluid leaked across the membrane and two tissue layers, reducing the volume of air in the other channel and compromising oxygen transport — just as it does in lungs of human patients when it is administered at the equivalent doses and over the same time course. Blood plasma proteins also crossed into the air channel, leading to the formation of blood clots in the air space, as they do in humans treated with IL-2.
But one result came as a surprise.
It turns out the physical act of breathing greatly enhances the effects of IL-2 in pulmonary edema — “something that clinicians and scientists never suspected before,” Ingber says. When the team turned on the vacuum attached to the chip to simulate breathing, it increased fluid leakage more than three-fold when treated with the clinically relevant IL-2 dose, and the Wyss team confirmed that the same response occurs in an animal model of pulmonary edema
This result could suggest that doctors treating patients on a respirator with IL-2 should reduce the tidal volume of air being pushed into the lungs, for example, in order to minimize the negative side effects of this drug.
Most exciting for the future of drug testing was the Wyss team’s finding that “this on-chip model of human pulmonary edema can be used to identify new potential therapeutic agents in vitro,” Ingber says. The pulmonary edema symptoms in the lung-on-a-chip disease model could be prevented by treating the tissues with a new class of drug, a transient receptor potential vanilloid 4 (TRPV4) channel blocker, under development by GlaxoSmithKline (GSK). In a separate study published by the GSK team in the same issue of Science Translation Medicine, the beneficial effects of TRPV4 inhibition in reducing pulmonary edema were independently validated using animal models of pulmonary edema caused by heart failure.
“In just a little more than two years, we’ve gone from unveiling the initial design of the lung-on-a-chip to demonstrating its potential to model a complex human disease, which we believe provides a glimpse of what drug discovery and development might look like in the future,” Ingber says.
“Organs-on-a-chip represents a new approach to model the structure, biology, and function of human organs, as evidenced by the complex breathing action of this engineered lung. This breathing action was key to providing new insight into the etiology of pulmonary edema,” said Dr. James M. Anderson, M.D., Ph.D., director of the NIH Division of Program Coordination, Planning, and Strategic Initiatives that provided partial support for this research through the Common Fund’s Regulatory Science program. “These results provide support for the broader use of such microsystems in studying disease pathology and hopefully for identifying new therapeutic targets.”
The work was funded by the National Institutes of Health (NIH) and the Food and Drug Administration (FDA), Defense Advanced Research Projects Agency (DARPA), and the Wyss Institute for Biologically Inspired Engineering at Harvard University.
original article by Kurzweil.ai
November 1, 2012
Movie List
Here's a listing of movies with a transhuman theme divided into fiction and non-fiction
Fiction
Matrix trilogy
2001;The space odessey
The terminator
Gattica
Avatar
Zardoz
Aeon flux
Bladerunner
Prometheus- Has the best promo website I've ever seen for a movie
Non-Fiction
Human v2.0: Making Gods
2057
Building Gods
Beyond Human: The Cyborg Revolution
Do you want to live forever?
Intelligence Revolution
Biotech Revolution
Quantum Revolution
Next World Series
Nanotopia
Transcendent Man
The Roots of the Matrix
The ATLAS Experiment
The Singularity Film
The Singularity is Near
The Meaning of the 21st Century
We Are The Singularity
Miracle Cure? A Decade of the Human Genome
The Power of Dreams
The Smartest Machine on Earth
Fiction
Matrix trilogy
2001;The space odessey
The terminator
Gattica
Avatar
Zardoz
Aeon flux
Bladerunner
Prometheus- Has the best promo website I've ever seen for a movie
Non-Fiction
Human v2.0: Making Gods
2057
Building Gods
Beyond Human: The Cyborg Revolution
Do you want to live forever?
Intelligence Revolution
Biotech Revolution
Quantum Revolution
Next World Series
Nanotopia
Transcendent Man
The Roots of the Matrix
The ATLAS Experiment
The Singularity Film
The Singularity is Near
The Meaning of the 21st Century
We Are The Singularity
Miracle Cure? A Decade of the Human Genome
The Power of Dreams
The Smartest Machine on Earth
Subscribe to:
Posts (Atom)
